CATARACT CLINIC
Cataract is the clouding of the eye’s natural lens. Cataract is one of the most common causes of vision loss in people.
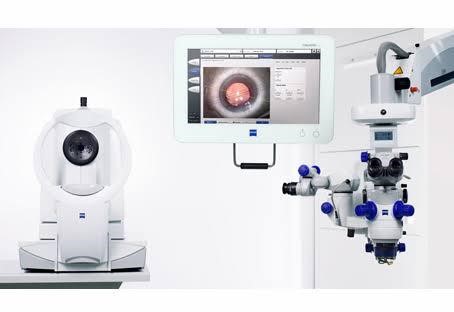
- High Precision Premium IOL surgery made fast and easy
- Precise and markless alignment of toric IOL’s
- Patient’s data injected into surgeon’s microscope for precision surgery
- Centration of IOL along the visual axis of the patient.
- Perfectly shaped, sized, and centered capsulorrhexis
- Helps to superimpose the exact position and size of incision to ensure precise surgery.
- The most common cause of cataract is ageing of the lens.
- An injury to the eye can also lead to cataract.
- Long term intake of steroids.
- Previous eye surgery.
- Exposure to harmful radiations.
- Systemic illness such as Diabetes, Hypertension, dehydration etc.
- Cloudy or blurred vision.
- Glare or light sensitivity.
- Fading or yellowing of colors.
- Double Vision in one eye.
- Poor night vision.
The only treatment of Cataract is surgical removal of cataractous lens with Intra Ocular lens implant.
Steps for Cataract Surgery
- Preoperative workup : Detailed slit lamp examination and dilated evaluation.
- Counseling : Patient is explained in detail about Cataract surgery and various IOL options available with the help of animations and videos.
- Medical checkup : Patient is advised to undergo blood test to assure fitness for the surgery.
- Surgical Procedure : Cataract surgery is a day care procedure with surgical time being 8 - 10 minutes and total stay in the hospital of about 2 - 3 hours.
- Post operative care: After the surgery patient and relatives are explained about the drops and care to be taken. Our staff takes special care to answer all the queries related to the surgery so that patient goes home stress free.
Amber eye care is equipped with latest diagnostic technology available for cataract surgery which includes Auto Keratometry, IOL master, SIRIUS from Germany for corneal topography, Potential Acuity meter (PAM), Zeiss OCT machine for macula evaluation, Palm scan in case of complicated cataract.
Infact it is one of the few centres to have all cataract diagnostic equipment under single roof.
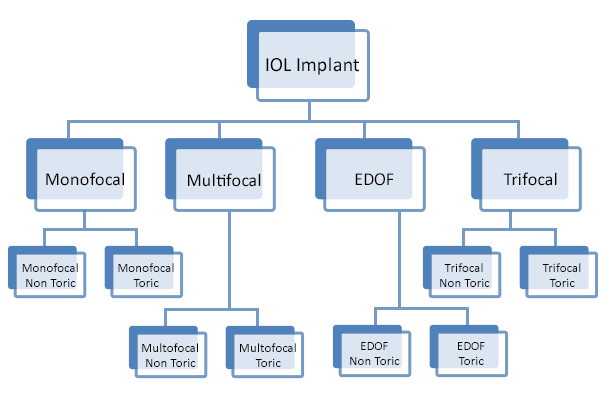
MICS (Micro - incision cataract surgery) or Micro - Phacoemulsification in which removal of the cataract is done through a 2mm incision with the implantation of foldable intraocular lens is a regular feature. All kinds of latest and advanced lenses are offered including foldable Trifocal lens, multifocal, the astigmatism correcting Toric IOLs and the combination of the two. The institute has advanced IOL measuring tools to reduce any measurement related errors such as the IOL master and the Immersion Biometry.
We believe in measuring twice and operating once. So all measurement are repeated multiple times on various devices so as to give optimal refractive results.
- No injection in eye.
- No sutures.
- No eye patch / dark glasses.
- Immediate Discharge.
- Limited post operative restrictions.
- Faster recovery.
- Minimal or no post op discomfort.
LASIK CLINIC
LASIK stands for Laser In - Situ Keratomileusis is a form of laser eye surgery that can correct a wide range of vision imperfections. The procedure is characterized by the creation of a flap in the cornea (the surface of the eye), before a computer - guided excimer laser is used to reshape the cornea to correct the patient's vision. The creation of the corneal flap improves results compared with traditional Custom Surface PRK ( Photorefractive Keratectomy ), and also helps to speed recovery and minimize discomfort.

ASA (Advanced Surface Ablation)
There are multiple methods of accomplishing ASA. It involves removing surface layer of cornea.i.e. epithelium( LASEK, Epi- LASIK, TransPRK) followed by excimer laser to re-shape the cornea.
TransPRK( No Touch No Flap) uses only laser to remove superficial layers.
It has less risk of long term corneal biomechanical instability and transient dry eye symptoms.
However ASA requires a longer healing process and is more likely to cause discomfort and irritation in initial 2-3 days following Laser Vision Correction.

CONTOURA
Contoura Vision is a topography - guided LASIK treatment that is the latest FDA approved LASIK eye surgery technology available. Contoura Vision can optimize the surface of the eye's cornea in such a way that it actually enhances the quality of vision better than has ever been possible before. In clinical studies, Contoura TMVision - Topography - Guided Laser Vision Correction helped 90% of patient's see as well or better without glasses than they did with glasses. It can benefit patient's in a number of ways, helping them obtain a better quality of vision and reducing the potential for night glare.

FEMTO LASIK (ALL LASER LASIK)
With All - Laser LASIK, we are able to create the corneal flap with extraordinary precision and without the need for a surgical blade. This typically makes the entire procedure virtually painless, while simultaneously giving our eye surgeons the ability to create a flap of precise thickness and shape. This can lead to enhanced visual outcomes and a more rapid healing process. Femto LASIK combined with Contoura treatment gives extraordinary accurate results while making the procedure even more safer.
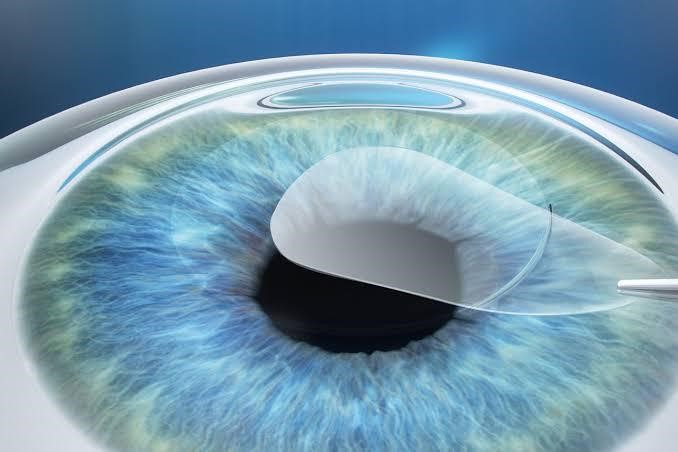
SMILE ( Small incision Lenticule Extraction)
Minimally invasive Laser Vision Correction procedure which uses Femtosecond laser with high precision and speed to reshape the cornea.
During the procedure a lenticule is created inside cornea which is subsequently extracted through a small incision of 2-4mm thereby achieving desired vision correction.
The preservation of upper corneal layers and the fewer transacted nerves may preserve biomechanical stability and reduce the incidence of transient dry eye symptoms.
LASIK is used to correct refractive errors, LASIK eye surgery is a treatment that reshapes the cornea in order to produce clear vision. The LASIK refractive eye surgery procedure can treat myopia (nearsightedness), hyperopia (farsightedness), astigmatism and reduce patient's dependency on contact lenses and glasses. Refractive errors impede the focusing ability of the eye, patient's who suffer from these conditions experience blurred vision. LASIK eye surgery provides these individuals with an effective treatment option, where a predetermined amount of corneal tissue is removed. This reshaping of the cornea improves the eye’s focusing power and enhances patient's visual acuity.
The number of people considering refractive surgery is at an all time high and LASIK is considered by virtually all refractive surgeons worldwide to be the procedure of choice today.
The following are some of the benefits of LASIK / Customized LASIK
- Simple to perform.
- Predictable.
- Stable.
- Brief recovery time.
- Minimal discomfort.
- Minimal post - op care.
- Low enhancement rate.
- Very low infection rate.
- Very low risk of scarring.
The results with LASIK are very stable and correction lasts for lifetime. In high powers, some residual power may remain or a slight regression may happen over a period of time. Are there any risks ? The chance of vision reducing complication is less than 1% and no sight threatening problems (loss of vision) are recorded. Some side effects like night glare, under correction rarely occur in very high powers. There is also a small possibility of regression especially in high powers. Infection is a remote possibility with every surgical procedure.
- The surgical procedure is relatively simple and takes only about 10 - 15 minutes for both the eyes.
- The anaesthetic drops are first instilled to cause numbing of the eye. This may give rise to a slight burning sensation as soon as the drops are instilled.
- A speculum (Clip) is placed to separate the eyelids and to prevent the patient from closing the eye during the procedure. The patient is asked to focus on a flashing red light.
- An instrument known as the microkeratome is then used to raise a thin flap (120 - 140µ) of the cornea. The red light may transiently disappear during this process. Alternatively the latest technique for making the flap is using a femto second laser (Zeimer) to make a highly precise and customized flap (90 - 100microns).
- The excimer laser then reshapes the cornea by removing a predetermined precise amount of tissue from the inner cornea. The flap is then repositioned back where it adheres immediately without the need for stitches or bandages.
- Visual recovery is full in 24 - 48 hours.
We believe in acquiring state of the art technology. The various equipments available for LASIK / Customized LASIK .
- Vario for corneal topography and Contoura treatment.
- Sirius for posterior float.
- Wavelight EX 500 excimer Laser from Alcon.
- Moria Microkeratome.
- Spectacle power assessment.
- Corneal topography using Sirius and Vario to assess the corneal thickness & curvature.
- Vario for customized Contoura LASIK.
- Peripheral retinal examination after dilating the pupillary aperture of the eye. The tests are mostly done on the day of the procedure.
- The entire preoperative assessment process may take about 1 - 2 hours. What is the surgical procedure for laser vision correction ?
- The surgical procedure is relatively simple and takes only about 10 - 15 minutes for both the eyes.
- The anaesthetic drops are first instilled to cause numbing of the eye. This may give rise to a slight burning sensation as soon as the drops are instilled.
- A speculum (Clip) is placed to separate the eyelids and to prevent the patient from closing the eye during the procedure. The patient is asked to focus on a flashing red light.
- An instrument known as the microkeratome is then used to raise a thin flap (120 - 140µ) of the cornea. The red light may transiently disappear during this process. Alternatively the latest technique for making the flap is using a femto second laser (Zeimer) to make a highly precise and customized flap (90 - 100microns).
- The excimer laser then reshapes the cornea by removing a predetermined precise amount of tissue from the inner cornea. The flap is then repositioned back where it adheres immediately without the need for stitches or bandages.
- Visual recovery is full in 24 - 48 hours.
DRY EYE CLINIC
Dry Eye Syndrome is very common condition affecting many people. It is a tear film disorder due to reduced production or excessive evaporation of tears which causes ocular discomfort. It can manifest in numerous ways such as burning sensation, pricking sensation, redness, feeling of heaviness in eyes, intolerance to contact lenses etc.
Risk factors associated with dry eyes included
- Aging
- Post menopausal status.
- Previous LASIK
- Patient on diuretics, beta blockers, psychotropics, oral acne medication
- Certain diseases like Rheumatoid Arthritis, thyroid disease, Steven Johnson’s syndrome, Ocular pemphigoid
- Contact Lens users
- Environmental factors like Air conditioning, low humidity
- Excessive screen time
Non-invasive Dry Eye Diagnostics –
TBUT – Non invasive Automated advanced analysis of Tear film breakup time. This test provides information on quality and quantity of patients tear film and thus helps in planning treatment.
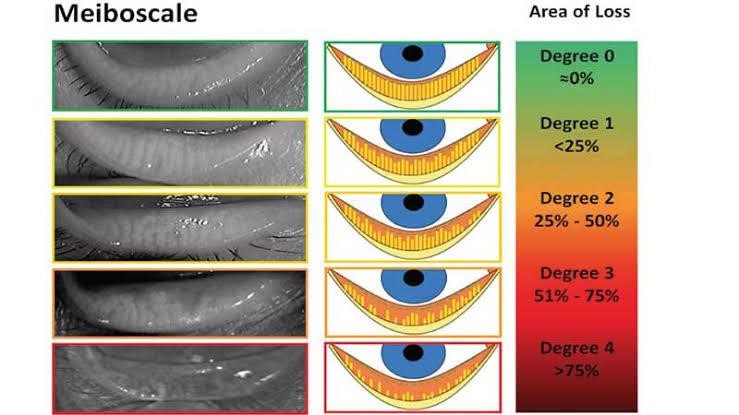
Meibography – Meibomian glands can be viewed under infrared illumination and can be then analysed to calculate gland health score. This gland health score will be indicative of severity of dry eyes and thus helps in planning the necessary treatment.

Dry Eye Treatment – Light Therapy
LIGHT MODULATION – LLT It’s a unique technology of photobiomodulation. The emission of a particular light to a certain wavelength triggers an endogenous heating of the eyelids .
This treatment eases the spill from the Meibomian glands stabilising the lipid layer of the tear film.
The treatment improves symptoms of the disease after few hours. Few sessions (2-4) at different intervals can be taken to achieve an optimal result.
GLAUCOMA CLINIC
Glaucoma is one of the most important cause of blindness in India, it is characterized by progressive damage to the optic nerve, this nerve acts like an electric cable with over a million wires. It is responsible for carrying images from the eye to the brain. Damage to optic nerve can result in vision loss. The most common cause accepted today is the increased intraocular pressure (IOP).
Glaucoma is a "silent thief" of sight as most of the times patient's do not experience any symptoms and are unaware of vision loss till severe damage has occurred. "Early detection and treatment of glaucoma by an ophthalmologist are the keys to preventing optic nerve damage and irreversible blindness".
(There are 2 major types of glaucoma : PRIMARY and SECONDARY. Open angle and angle closure are the most common forms of the disease).
Glaucoma Causes
Glaucoma can be caused by increased pressure of the fluid in the eye. The inside of the eye contains fluid that is constantly flowing into and being drained out of the eye. If the drainage mechanism in an area called Trabecular meshwork gets blocked, fluid starts accumulating in the eye, exerting pressure inside the eye. This extra fluid that builds up in the eye presses against the optic nerve at the back of the eye, thus damaging parts of the optic nerve. This damage appears as gradual visual changes and then loss of vision, if it remains untreated.
Chronic Open Angle Glaucoma : The most common type of glaucoma, known as chronic open angle (COAG) or primary open angle, occurs when the canals draining the eye of aqueous humour become clogged. This blockage can gradually increase pressure within the eye to damaging levels. No pain occurs, so individuals are usually unaware that these changes are occurring. There are no early signs or symptoms but over the years vision will be lost starting in the periphery and moving towards the central vision.
Acute Angle Closure Glaucoma : When eye pressure builds up rapidly, it is called acute angle - closure glaucoma. This type of glaucoma commonly occurs in individuals who have narrow anterior chamber angles. In these cases, aqueous fluid behind the iris cannot pass through the pupil thus pushing the iris forward, preventing aqueous drainage through the angle. It is as though a sheet of paper floating near a drain suddenly drops over the opening and blocks the flow out of the sink. In cases of acute angle closure glaucoma, one may experience blurred vision, halos around lights, deep pain behind the eye, nausea, and vomiting.
- Family members with glaucoma.
- Age more than 40 years.
- People who has Diabetes.
- Myopia (nearsightedness).
- Regular, long term steroid / cortisone use.
- A previous history of TRAUMA.
- High blood pressure.
- Thyroid disorders.
- Humphrey visual field analyser.
- Optical coherence tomography for RNFL analysis.
- Scheimpflug analysis for the anterior chamber and angle analysis.
- Pachymetry, non contact tonometry and ONH photography.
Being a silent disease, glaucoma has no symptoms in its early stages, and vision remains normal. Patient is usually unaware until the optic nerve is badly damaged. Because of lack of symptoms, the best way to diagnose this form of glaucoma is by detailed and periodic eye examination.
Common Symptoms
- Headache.
- Eye pain.
- Blurred vision.
- Redness / watering of eyes.
- Colored halos.
- Nausea and vomiting.
In presence of any of these symptoms, visit your ophthalmologist immediately. Unless the type of glaucoma is treated early, blindness can occur.
Aim of the treatment is to prevent further damage.
Medical Treatment
- Glaucoma is usually controlled with eye drops taken daily, they lower the eye pressure either by slowing the formation of aqueous fluid within the eye or by increasing the flow at the drainage area.
- Maintain proper timing of application suggested by your doctor.
- Do not change or stop taking your medications without consulting your ophthalmologist.
- If you are about to run out of your medications, ask your ophthalmologist if you should have your prescriptions refilled.
Modalities of treatment
Surgery
Treatment depends on the stage of the disease at presentation. Appropriate and early treatment can prevent the loss of sight in majority of patient's. The aim of treatment is to allow the patient to lead an independent and fully functional lifestyle. Because glaucoma can progress without your knowledge, adjustments to your Glaucoma treatment may be necessary from time to time.
Laser treatment
Open - angle glaucoma the draining angle itself is enlarged to control eye pressure. Angle - closure glaucoma the laser creates a hole in the iris to open up and improve the flow of aqueous fluid to the drain.
Newer LASER (Selective Laser Trabeculoplasty).
- Applanation tonometer : This is one of the most accurate ways to measure the eye pressure.
- Gonioscope : Used to study the angle between the cornea and iris in patient's, suspected or having glaucoma.
- Computerized visual field analyzer (automated perimeter) : A computerized instrument used to map the field of vision, managing glaucoma & diagnosis of various neurological conditions.
- Optical Coherence Tomography (OCT) : This is a diagnostic procedure similar to the CT scan of the brain. It uses a beam of light and its reflection to obtain cross - sectional images that provide information about the different layers of the retina.
RETINA CLINIC
The vitreoretinal centre in Amber eye care is well equipped with state - of - art imaging and diagnostic facilities which deals with the management of all retinal disorders like diabetic retinopathy, ARMD, retinal detachment, trauma, infections and other retinal disorders.
We aspire to provide highest quality medical and surgical care for our patient's with retinal diseases in a compassionate and efficient environment. Retinal related surgery is an extremely specialized and skilled area of practise. At Amber eye care we have a dedicated team of specialists handling vitreoretinal disorders. Our doctors are well trained with surgical and diagnostics skills for treating such specific retinal problems.
Common Diagnostic Tests at Amber eye care
- Fundus Photography : Color photographs of the Retina at the back of the eye.
- Fluorescein Angiography (FFA) : A diagnostic procedure that photographs the blood circulation of the retina. This involves injection of a dye called fluorescein into a vein in the arm or hand.
- Optical Coherence Tomography (OCT) : This is a diagnostic procedure similar to the CT scan of the brain. It uses a beam of light and its reflection to obtain cross - sectional images that provide information about the different layers of the retina.
- Visual Field Analysis (Perimetry) : Measurement of the full extent of the area visible to an eye that is fixating straight ahead.
- Ultrasonography of eye (B - Scan) : This is a diagnostic test used to produce a two - dimensional, cross - sectional view of the eye to assess posterior segment of the eyeball when media is hazy due to cataract or any corneal opacity.
Diabetic Retinopathy
Diabetic retinopathy is an eye problem that can be caused by either type 1 or type 2 diabetes mellitus. Retinopathy occurs when diabetes damages the tiny blood vessels in the retina which may leak fluid and blood. It’s a sight threatening condition, however if diagnosed and treated, vision loss can be prevented. Firstly, examination of the retina of the eye is done using indirect ophthalmoscopy after dilating the pupils. If diabetic retinopathy is found, specialized test.
- OCT (Optical coherence tomography).
- Fluorescein angiography (FFA).
These tests will help us in deciding the stage & treatment of Diabetic Retinopathy.
Laser Treatment : The aim of this treatment is to protect central vision. It does not restore lost vision, but it can prevent further deterioration, which is why early diabetic retinopathy diagnosis through periodic eye examination is imperative.
Intravitreal Injections (Anti VEGF agents) : Anti VEGF agents (Accentrix, Avastin, Eylea) are emerging as the new modality of treatment for various stages of diabetic retinopathy. These agents are injected into the eye (intravitreal injection). They are commonly used in diabetic maculopathy and proliferative diabetic retinopathy.
Surgery (VITRECTOMY) : A microsurgical procedure where the blood filled vitreous gel is replaced with a clear gas / solution / oil to restore vision.
Age - Related Macular Degeneration (ARMD)
Age - related macular degeneration (ARMD) is the most common cause of irreversible vision loss in people over age of 60 years. Cells in the macula degenerate (the central, and most sensitive part of the retina at the back of the eye) that is, they become damaged and die. Damage to the macula affects your central vision which is needed for reading, writing, driving, recognizing people's faces and doing other fine tasks.
Types of ARMD
ARMD is of two types
- Dry ARMD – (90%) : LESS SEVERE.
- Wet AMD – (10%) : MORE SEVERE.
Vision loss is usually gradual. These patient's need to monitor their central vision regularly. If you notice any change in your vision, you should tell your eye doctor right away, as the dry form can change into the more damaging form which is wet (exudative) macular degeneration. While there is no medication or treatment for dry macular degeneration, some people may benefit from vitamin supplements (anti - oxidants).
This can cause more damage to your central vision than the dry form. Wet macular degeneration occurs when abnormal blood vessels begin to grow underneath the retina. This blood vessel growth is called choroidal neovascularization (CNV) because these vessels grow from the layer under the retina called the choroid. These new blood vessels may leak fluid or blood, blurring or distorting central vision. Vision loss from this form of macular degeneration may be faster and more noticeable than dry AMD.
- Blurred or distorted central vision.
- Colors look dim.
- Words on a page look blurred.
- Straight lines appear distorted.
- Dark or empty areas appear in the center of vision permanent loss of your central vision.
Diagnosis
- Dilated retinal examination.
- Amsler Grid : To detect defects in central vision.
- Fundus Fluorescein Angiography(FFA).
Treatment
There is NO TREATMENT for dry AMD, although high dose multivitamin combination has been shown to decrease the risk of visual loss. There are a few treatment options for wet AMD although the best outcomes occur when this disease is detected early.
- Laser.
- Photodynamic therapy (PDT).
- Anti - VEGFs (Accentrix, Avastin, Eylea).
- Combinations of the above mentioned Not all patient's may benefit from these, and treatment may not prevent further vision loss.
Retinal Detachment
The RetinaThe retina is a nerve layer at the back of the eye that senses light and sends images to the brain.
Meaning of Retinal DetachmentThe retina is the light - sensitive layer of tissue that lines the inside of the eye and sends visual messages through the optic nerve to the brain. When the retina detaches, it is lifted or pulled from its normal position. If not promptly treated, retinal detachment can cause permanent vision loss.
Risk- High Myopia (near - sightedness).
- Injury to the eye.
- Previous retinal detachment in the other eye.
- Family history of retinal detachment.
- Areas of thin / weak retina.
Symptoms
- Floaters which are little "cobwebs".
- Light flashes in the eye.
- Sudden blurry vision.
- An area of dark vision, like a curtain or a veil coming from above or below or from the sides. Floaters are a common symptom in otherwise normal individuals. However if these are accompanied by persistent flashes, they could be symptoms of a retinal tear or detachment.
Treatment
Retinal tears without detachment - Laser photocoagulation or cryotherapy is performed around the tear to seal the retina to the back wall of the eye.
Retinal tears with retinal detachment - Requires surgery as soon as possible to put the retina back in its proper position. The longer the retina stays detached, the less the visual improvement after surgery. Scleral buckle surgery - A flexible silicone band is placed around the eye to counter the force pulling on the retina after removing the fluid under the detached retina.
Lasers
Indirect Ophthalmoscopic Laser Delivery System (LIO) : This laser delivery system is mainly used for peripheral retinal lesions
- Horse shoe tear (HST).
- Lattice degeneration.
- Retinal holes.
- Retinopathy of prematurity (ROP).
- Pan retinal photocoagulation for vascular retinopathy in a hazymedia.
- Cryotherapy: is a second way of treating retinal tears apart from laser. An extremely cold probe is used to "freeze - burn" a small area on the outside of the eyeball that overlies the retinal tears. The purpose is to seal the tears and create an eventual scar that will "stick" the retina to that spot.
- Pneumoretinopexy:is a method of treating selected cases of retinal detachments. A gas bubble is injected into the eye after applying cryo spots to the area of retinal tear.
Vitrectomy
In the event of the patient presenting with very advanced diabetic retinopathy, a microsurgical procedure known as vitrectomy is recommended. Blood - filled vitreous gel of the eye is replaced with a clear solution to aid in restoring vision. Sometimes the retina may also be detached. Vitrectomy surgery is then performed to reattach the retina.
Sutureless Vitrectomy Points to Remember
- Control your blood glucose as effectively as possible.
- Keep your regular screening appointment.
- Get advice if you have a problem with your sight.
- Check your cholesterol levels regularly.
- Stop smoking.
CORNEA CLINIC
The human eye has 3 coats, the outermost of which is protective fibrous layer, the sclerocorneal layer. The sclera is the white of the eye. Placed in the front of the sclera, like a watch glass, is the CORNEA.
The cornea is a transparent structure and the window through which we see the world. It accounts for a major part of the refractive power of the eye and is primarily responsible for focusing light rays on to the retina of the eye.
The diseases which affect the cornea and cause loss of transparency include Corneal Infections, Corneal degenerations, corneal thinning disorders like Keratoconus. Injuries (mechanical trauma / chemical burns) are also one of the most common causes for corneal blindness.
Keratoconus
Keratoconus is a disease where the cornea becomes thinner than normal, and subsequently starts bulging forward. This causes a blurring of visual images and is a known progressive condition. It is a disease of youngsters, starts in the second decade and is commoner with childhood eye allergy and rubbing habit. It causes frequent change of glasses with increase in cylindrical power. Keratoconus is treated in earlier stage with semi - soft contact lenses, but such lenses would not slow the disease process.
Now, there are a lot of advances in keratoconus treatment. One of the recent treatments is Corneal Collagen Cross - linking with Riboflavin) C3R, (which is a procedure that aims to stabilize a keratoconic cornea. Kerarings are implantable rings inserted into the cornea to flatten the corneal cone, and thus, also helps to improve vision of the patient. We can even put special Implantable contact lenses called Toric ICL to improve vision further in these cases.
Corneal trauma
Injury to the cornea is potentially blinding, and may be minor such as a small superficial foreign body, or major, such as acid / alkali) lime (burns or penetrating injury. emergency treatment is mandatory in any kind of injury to the eye. for chemical injuries, one should immediately wash eyes thoroughly with plenty of water for half an hour and immediately see an eye doctor.
Corneal Infections
A corneal ulcer is an open sore in the cornea. It is usually produced by an infection, commonly bacterial, fungal or viral. The ulcer can either be located in the centre of the cornea, greatly affecting the vision or in the periphery not affecting the vision.
Infections that develop in the cornea are frequently associated with trauma, contact lens overuse and dry eyes. It causes pain, redness and watering in the eye which can be quite severe. Ulcers frequently require 2 - 3 months of intensive treatment with eye drops and / or tablets and heal by corneal scarring. If visual loss occurs, this may require corneal grafting later in future. If medical treatment fails, intense suppuration (pus formation) often ensues, and the cornea can eventually perforate. Hence non healing ulcers may require therapeutic corneal grafting to save the eye.
- Corneal topography.
- Ultrasound pachymeter.
- Scheimpflug analyser.
- Meibography.
- C3R.
- Smart plugs for dry eyes.
- Corneal tattooing.
Comprehensive Eye Examination
A Routine Eye Examination includes testing of Vision, Recording eye pressure, refraction by an optometrist and evaluation of anterior and posterior eye structures. For examination of retina and other posterior structures of eye a dilating drop is instilled in patient’s eyes which take its action in 20 – 30 minutes and the effect remains for 3 to 4 hours.
The complete examination requires 45 to 60 minutes.
At Amber eye care all types are contact lenses are available including speciality contact lens used for patients with corneal disorder resulting in corneal irregularities like Keratoconus.
Low vision aids clinic offers rehabilitative services to patients with low vision in the form of various optical magnifiers, telescopes and electronic low vision aids.
Amber eye care provides comprehensive clinical care to a broad spectrum of cases including optic neuritis, ischemic optic neuropathy, compressive optic neuropathy (including pituitary tumors), papilledema, inflammatory and infectious optic neuropathies, cerebrovascular disorder or tumors involving vision, ocular motor disorders (including cranial nerve palsies), hereditary and traumatic optic neuropathies which can result in decrease in central vision, disorder of the visual field, double vision (seeing double due to misalignment of the eyes with abnormal eye movements), abnormal drooping of eyelids, severe headache, which may or may not be associated with intermittent blurring of and vomiting.
Patients who are bedridden or handicapped are seen by an optometrist visiting them at their residence. A detailed examination is done by him/her. If there is something that need ophthalmologist’s attention patient is advised accordingly.
OCULOPLASTY CLINIC
The Orbit and Oculoplasty speciality deals with the management of diseases and abnormalities of the orbit, eyelids and the lacrimal system. Common surgeries done at our centre are
Eyelid surgery
Eyelids can have a variety of deformities such as droopy eyelids, eyelid bags, puffy eyelids, in - turned eyelid margins. Children are sometimes born with droopy eyes – this condition is called congenital ptosis and if the lid droop is very severe especially in young children, it can even lead to lazy eye (amblyopia).Orbital Surgery
The orbit refers to the bony socket inside which the eyeball and the muscles (extraocular muscles) are situated. Orbital surgeries involves surgeries to repair the trauma of the bony orbit, to remove tumours situated behind the eye, enucleation surgeries and evisceration ( procedures used to remove a diseased eye) following which surgical reconstruction and ocular prosthesis is done to improve cosmetic appearance.Lacrimal surgery
The lacrimal system largely consists of the lacrimal gland that produces tears which moisten the surface of the eye and the “ducts” or tubes that drain tears from the eye into the nose. The most common symptoms of lacrimal system problems include watering or excess tearing (to the point that tears might run down the face) and mucous discharge. Common problems include blockage of the nasolacrimal duct for which Syringing / irrigation, nasolacrimal duct probing, Dacryocystorhinostomy, Endonasal dacryocystorhinostomy and Dacryocystectomy procedures can be done.Facial Aesthetics
Aesthetic surgery refers to all procedures done to enhance the beauty of the face.
Procedures performed include lid - lift ( to correct aging, sagging eyelids and to correct the excess hooding of skin on the upper lids), lower lid blepharoplasty (to correct the lower eye lids bags and fat prolapse). Botulinum tox (Botox) injection is also given to smoothen fine lines or wrinkles. Dermal fillers are substances which are injected into the skin to help fill in the wrinkles and thereby restoring a smoother appearance. They not only smoothen but also add volume to the face. A combination of two or more procedures can be done to obtain a remarkable youthful look which is strikingly beautiful and natural.
PAEDIATRIC CLINIC
The Paediatric clinic deals with any eye conditions that affect children in form of Refractive error, Amblyopia (Lazy eye), Cataract, ROP, Squint or Misaligned or Cross eye in Children / Adult. There are many eye conditions affecting children which may be present at birth or occur later in childhood. Some of the common problems occurring in children are
It is most common problem in children which usually go unnoticed if present in one eye. Most of the Refractive errors occur during early childhood and can lead to ‘Lazy eye’. Hence an early eye examination becomes necessary for all the children.
Common complains (Symptoms)
- The child may complain of blurred vision or may make mistakes in his / her note books.
- Asthenopic Symptoms (Headache, Blurring of vision).
- Goes close to blackboard / Television to see.
- Squeezing / Rubbing / Blinking eyes more frequently.
Tests done
- Refraction performed by an optometrist / ophthalmologist is helpful in tests done of refractive error.
Treatment
- Glasses are the most common means of correcting refractive errors.
- Contact lens and Refractive surgeries are not preferred for children.
Squint, also known as strabismus, is a condition where both the eyes do not look together in the same direction. So if one of your eyes looks straight ahead, the other turns to point inwards, outwards, upwards or downwards. Squint may even appear occasionally or seen constantly. It can cause Lazy eye / Amblyopia in one eye.
Common complains (Symptoms)
- Generally there no Symptoms when the deviation is large. However, Patient may complain of headache, eyestrain or sensitivity to light if the deviation is small.
- Parents / Relatives may notice the misalignment of eyes.
Tests done
- Complete eye examination along with cover / uncover test and other special tests are required for testing squint.
- Early Tests done is helpful in giving better treatment of squint.
Treatment
- Squint is treated with glasses, prisms or surgery for alignment of eye muscles. Sometimes a combination of all these may be required.
Any cloudiness of the normally transparent lens is referred to as a cataract. Although it occurs naturally as an ageing process in adults it is not uncommon for children to have cataract. Cataract can be present at birth which is called ‘congenital cataract’ or it may develop later in life. It may be inherited or may occur as a result of infection, inflammation, injury or as a developmental abnormality. It may be seen in one or both the eyes.
Common complains (Symptoms)
- White spot may be visible in the pupillary area.
- Patient may complain of blurred vision.
- Misalignment of one eye (the eye with cataract).
Tests done
- Cataract is diagnosed during comprehensive eye examination by an ophthalmologist.
Lazy eye or amblyopia is the term for poor vision in one or both eyes. It can result from refractive error, squint or several other causes. It needs to be identified and treated at an early age to recover vision.
Common complains (Symptoms)
- Generally there are no specific symptoms of amblyopia, but the child may present with symptoms associated with causative disorder e.g. refractive error, Squint.
Tests done
- It is detected by vision screening and refraction done at eye clinics.
Treatment
- Firstly, the condition that is responsible for causing poor vision in the lazy eye needs to be treated for which glasses may be prescribed or patient may have to undergo surgery ( e.g. Squint, Cataract).
- Patching therapy i.e. patching the good eye is given to improve the vision of the Lazy eye. It usually takes some months for the vision to improve although it depends on various factors.
- Patching therapy is effective till the age of 8 to 9 years although this may vary for some patient's.
Retinopathy of Prematurity (ROP) is an eye disease seen in premature babies in which there is growth of abnormal blood vessels on their retina. ROP usually affects the youngest, smallest and sickest of infants. The more premature and the smaller your baby is, the higher the chances of developing ROP.
Factors warranting an examination to rule out ROP
- White - looking pupils.
- Abnormal movements of the eye.
- Crossed eyes.
- Low Birth weight (<2100 gms).
- Low gestational age (born before 35 weeks).
- Use of supplemental oxygen after birth.
What are the Tests to diagnose ROP ?
- Child needs detailed retinal evaluation after dilating eye. Timely examination is of utmost importance to prevent loss of vision before it becomes too late.
What are the Treatment options for ROP ?
ROP is divided into 5 stages according to the severity.
If the ROP is in the early stages (1 and 2), no treatment is required as it usually gets better on its own.
If the condition has advanced to stage 3 or beyond treatment is needed. Infants are treated at about 32 – 40 weeks. The following options are available
- Laser treatment (photocoagulation) is used to eliminate the abnormal blood vessels.
- Cryotherapy (freezing to prevent the abnormal blood vessels from spreading).
- Eye glasses.
- Eye drops.
- Patching one eye ( if amblyopia has to be treated ).
- Scleral Buckling (placing a band around the eyeball) or Vitrectomy (removal of the gel inside the eye) surgery may be needed if the condition has reached stage 4 or 5 and retinal detachment has occurred.
LOW VISION CLINIC
For patients who are not able to see clearly with normal/usual glasses or contact lenses, Amber Eye care has specialised devices which help them in doing their day to day activities like watching television, reading newspaper/books, using computers, etc. These devices can help you make the most of your vision so that you can perform everyday tasks more easily and with less frustration.
Guidance for availing Low vision devices
- Low vision evaluation is conducted by our consultant optometrist.
- Based on patient’s needs different aids are tried
- After the evaluation, devices are recommended to the patient which best suits their needs
- We order the device for the patient which he/she is interested in availing.
- As the patient uses the device he/she learns more about it and is able to use it more conveniently.
022-25398811 , 022 25398844 , 022 25398855